Every year, tens of thousands of people end up in the emergency room not from a car crash or fall, but from something most of us keep in our medicine cabinets: acetaminophen. It’s in Tylenol, Excedrin, NyQuil, Sudafed, and over 600 other OTC and prescription meds. You think you’re being careful-just one or two pills for a headache. But if you don’t know what you’re taking, or how much is safe, you could be quietly damaging your liver.
Why Acetaminophen Is the Silent Threat
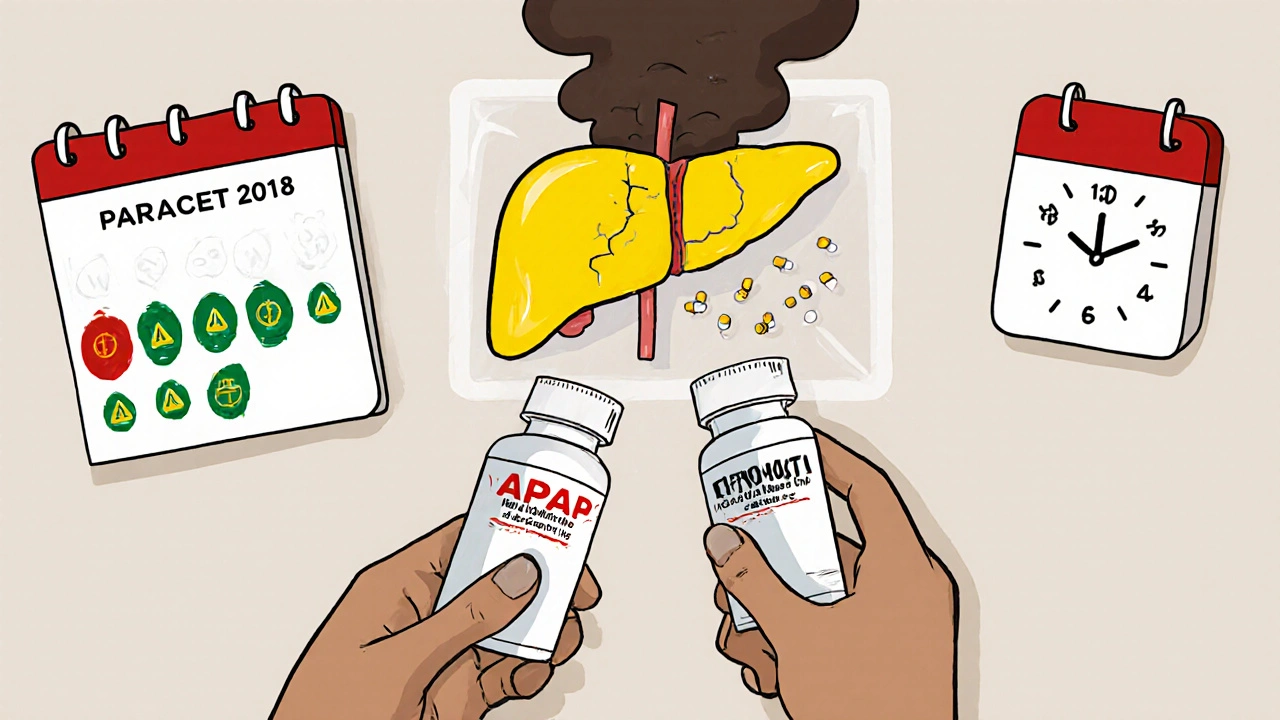
Acetaminophen is not dangerous because it’s toxic by nature. It’s safe when used correctly. The problem is how easy it is to accidentally take too much. Your liver breaks down acetaminophen into harmless waste-but when you hit a certain dose, usually above 4,000 mg in 24 hours, it starts producing a toxic byproduct called NAPQI. Your liver normally neutralizes this with glutathione, but if you’ve taken too much, that buffer runs out. Then, NAPQI starts killing liver cells.
This isn’t theoretical. According to the CDC, acetaminophen causes about 56,000 emergency visits, 26,000 hospitalizations, and nearly 500 deaths each year in the U.S. Most of these aren’t suicide attempts. They’re mistakes. Someone takes a Tylenol for a headache, then takes a cold medicine that also has acetaminophen. Or they take extra-strength pills all day because the regular ones didn’t work. Or they drink alcohol while taking it-something many people don’t realize makes the danger much worse.
How Much Is Too Much?
The FDA says 4,000 mg per day is the max for healthy adults. But that number isn’t the same for everyone.
- If you have fatty liver disease, hepatitis, or cirrhosis, your limit drops to 2,000 mg per day.
- If you drink alcohol regularly-even just a glass or two a day-your safe limit is also 2,000 mg or less.
- If you’re underweight, elderly, or taking other medications that affect liver function, talk to your doctor before taking more than 3,000 mg daily.
And here’s the catch: a single extra-strength Tylenol tablet is 500 mg. Four of them get you to 2,000 mg. That’s half the max for a healthy person-and it’s the full limit for someone with liver issues. Many people don’t realize how fast those pills add up.
Hidden Acetaminophen Is the Biggest Risk
You won’t always know you’re taking it. Acetaminophen is added to dozens of cold, flu, allergy, and sleep aids. If you’re taking more than one OTC product at a time, you’re likely doubling up without realizing it.
According to the FDA, about 25% of unintentional acetaminophen overdoses happen because people combine cold medicines with pain relievers. You take DayQuil for your stuffy nose, then take Tylenol for your fever. Both have acetaminophen. You think you’re helping yourself. Instead, you’re pushing your liver past its limit.
Always check the “Active Ingredients” section on the label. Look for these names:
- Acetaminophen
- Paracetamol
- APAP (that’s the chemical abbreviation)
If you see any of these in more than one product, don’t take them together. Even if one says “non-drowsy” and the other says “nighttime,” they can still have the same active ingredient.
NSAIDs Aren’t the Safe Alternative You Think
People often switch to ibuprofen or naproxen thinking they’re safer for the liver. That’s partially true-but it’s not the whole story.
NSAIDs like Advil, Aleve, and Motrin don’t cause liver damage the way acetaminophen does. But they’re hard on your stomach, kidneys, and heart. Diclofenac, in particular, has been flagged by the FDA as one of the most likely NSAIDs to cause rare but serious liver injury. And if you already have liver disease, NSAIDs can make kidney problems worse-something that’s already common in people with cirrhosis.
So what’s the best choice? For people with liver disease, acetaminophen at low doses (2,000 mg or less) is still considered safer than NSAIDs. But only if you’re not drinking alcohol and you’re not taking other liver-affecting meds.
What to Do Instead
If you’re managing chronic pain-back pain, arthritis, headaches-you don’t have to rely on pills. Non-drug options work better and are safer long-term.
- Physical therapy improves mobility and reduces pain without drugs.
- Cognitive behavioral therapy helps change how your brain processes pain signals.
- Acupuncture has been shown in multiple studies to reduce chronic pain, including osteoarthritis and migraines.
- Topical creams like diclofenac gel (Voltaren) deliver pain relief directly to the skin, with almost no liver exposure.
These aren’t quick fixes, but they’re sustainable. And they don’t risk your liver.
Signs Your Liver Is Under Stress
Acetaminophen damage doesn’t always hurt right away. By the time you feel sick, it might already be serious.
Watch for these symptoms within 24 to 72 hours after taking too much:
- Nausea or vomiting
- Loss of appetite
- Extreme tiredness
- Pain in the upper right side of your abdomen
- Dark urine
- Clay-colored stools
- Yellow skin or eyes (jaundice)
If you notice even one of these after taking OTC pain relievers, get medical help immediately. Don’t wait. The antidote, N-acetylcysteine (NAC), works best if given within 8 hours of overdose. After 16 hours, its effectiveness drops sharply.
How to Protect Yourself
Here’s a simple plan to avoid liver injury from OTC pain relievers:
- Know your dose limit-4,000 mg max for healthy adults, 2,000 mg if you have liver disease or drink alcohol.
- Read every label-look for acetaminophen, paracetamol, or APAP in every pill you take.
- Never combine-if you’re taking a cold medicine, don’t also take Tylenol.
- Avoid alcohol-even one drink can double your risk of liver damage.
- Use a pill organizer-set daily limits with a marker or sticker so you don’t lose track.
- Track your meds-write down everything you take, including supplements. Many people forget herbal products can affect the liver too.
- Ask your pharmacist-they can scan your meds and tell you if you’re at risk.

What’s Changing in 2025
Regulators are catching up. Since 2022, all OTC acetaminophen products in the U.S. must have a clear “Liver Warning” on the front label and bold text saying “Do Not Exceed 4,000 mg Daily.” That’s helped reduce accidental overdoses by 21%, according to Johns Hopkins.
There’s also new research into genetic testing. Some people have a variation in the gene that makes glutathione-the liver’s natural defense. These people are more sensitive to acetaminophen and may need to cap their intake at 2,000 mg even if they’re otherwise healthy. Companies like 23andMe now offer tests that can identify this risk.
And the NIH is investing $47 million over the next few years to develop new painkillers that don’t go through the liver at all. That’s the future-but for now, awareness is your best protection.
What to Do If You’ve Taken Too Much
If you think you’ve taken more than your limit-even if you feel fine-call Poison Control at 1-800-222-1222 immediately. Don’t wait for symptoms. Don’t try to “sleep it off.” Don’t assume you’re fine because you didn’t take 10 pills at once.
Unintentional overdoses happen slowly. One extra pill here, one cold medicine there. By the time you feel bad, your liver may already be in trouble. The antidote works best early. Time matters.
Can I take Tylenol if I have hepatitis C?
Yes-but only up to 2,000 mg per day, and never with alcohol. Even mild liver damage from hepatitis C makes you more vulnerable to acetaminophen toxicity. Always check with your doctor before taking any pain reliever.
Is it safe to take acetaminophen with ibuprofen?
Yes, if you stay within limits. You can take 325 mg of acetaminophen and 200 mg of ibuprofen together, as long as neither exceeds your daily maximum. But don’t take combination products that already contain both. Always space doses at least 4-6 hours apart.
Does NAC (N-acetylcysteine) work as a supplement to prevent liver damage?
No. NAC is only effective as a medical treatment given in a hospital within hours of an overdose. Taking it daily as a supplement doesn’t protect your liver from acetaminophen damage. It won’t help you take more pills safely.
What’s the safest OTC pain reliever for someone with a fatty liver?
Acetaminophen at 2,000 mg or less per day is still considered the safest option for people with fatty liver disease. NSAIDs like ibuprofen carry higher risks for kidney and stomach problems in this group. Always avoid alcohol and talk to your doctor before starting any new medication.
Can children take acetaminophen safely?
Yes, but only at the correct weight-based dose. Pediatric dosing is different from adult dosing. Always use the measuring device that comes with the medicine, never a kitchen spoon. Since 2019, public awareness campaigns have reduced pediatric acetaminophen poisonings by 35%.
Are natural supplements like turmeric or CBD safer for the liver?
Some supplements, including high-dose turmeric and CBD, have been linked to rare cases of liver injury. Just because something is “natural” doesn’t mean it’s safe for your liver. Always talk to your doctor before using supplements, especially if you have liver disease.
Final Takeaway
OTC pain relievers are convenient. But convenience shouldn’t override caution. Acetaminophen is one of the most common drugs in American homes-and one of the most dangerous if misused. You don’t need to avoid it entirely. You just need to know how much you’re taking, what else you’re mixing it with, and when to say no. Your liver doesn’t have a voice. But you do. Use it wisely.
12 Responses
I had no idea acetaminophen was in so many cold meds. I took NyQuil last week for my cold and then took Tylenol for my headache-turns out I was doubling up. Yikes. 😅 Now I always check the labels. Learned the hard way.
People treat medicine like candy. ‘It’s over-the-counter, so it’s harmless.’ No. Your liver isn’t a trash compactor. You don’t get bonus points for ‘just a little extra.’ This isn’t a game. Stop being reckless and start reading labels-or don’t complain when your organs fail.
So… if I take one Tylenol and then a DayQuil that also has it, I’m basically doing a liver suicide pact? Cool. Got it. 🙃
Great breakdown! I’m a nurse and I see this all the time-people don’t realize how sneaky acetaminophen is. I always tell my patients: if it’s for sleep, cold, or pain, assume it has APAP unless proven otherwise. And please, PLEASE don’t mix with alcohol. I’ve seen 22-year-olds with acute liver failure because they had a beer with their cold meds. 😢 It’s preventable. Knowledge saves lives.
As a British citizen, I find it appalling that American OTC regulations are so lax. In the UK, paracetamol is sold in blister packs of 16 tablets max, and pharmacists are required to advise on dosage. Here, you can buy a bottle of 500 pills with no oversight? Madness. This is why the U.S. has such high rates of iatrogenic harm. The FDA’s 2022 label changes are a start-but not nearly enough.
Oh wow, so I’ve been poisoning myself for years? 😂 I take 2 extra-strength Tylenol every night with my whiskey. ‘It helps me sleep.’ Turns out it helps my liver… exit stage left. Thanks for the heads-up, doc. Now I know why my bloodwork’s been weird.
Read the label. Don’t mix. No alcohol. Done. Why is this so hard?
It’s funny how we’ll spend hours researching the best coffee maker but won’t read the back of a pill bottle. We treat our bodies like disposable gadgets. ‘It’s just one more.’ But your liver doesn’t have a reset button. Maybe the real problem isn’t acetaminophen-it’s our culture of ‘I’ll figure it out later.’
Let’s be real: 90% of these ‘accidental overdoses’ are just people who don’t want to admit they’re addicted to painkillers. You don’t ‘accidentally’ take 8 pills in a day. You just call it ‘accidental’ because you’re ashamed. Stop lying to yourself. Get help. Or stop pretending you’re innocent.
As a woman with autoimmune liver issues, I’ve been told by three different doctors to stick to 2,000 mg max. But my husband says, ‘You’re fine, you’re young!’ Then he hands me Tylenol for my migraines. I’m not ‘fine.’ I’m one wrong pill away from a transplant. This isn’t just ‘information’-it’s survival.
One critical point missing: many herbal supplements-milk thistle, green tea extract, kava, and even high-dose turmeric-have been linked to hepatotoxicity. While acetaminophen is the most common cause of acute liver failure, natural products are rising in incidence. Always disclose ALL supplements to your provider. The assumption that ‘natural = safe’ is dangerously false. Document your intake. Consult a pharmacist. Your liver will thank you.
Acetaminophen is the NSAID of the 21st century: ubiquitous, misunderstood, and quietly murdering people who think they’re being smart. Meanwhile, Big Pharma markets it as ‘gentle’ while burying the fine print in 6-point font. The real villain isn’t the drug-it’s the corporate lie that ‘safe when used as directed’ means ‘safe when used as you want.’ Wake up. Your liver isn’t a vending machine.