That sharp, electric shock of pain shooting down your arm or leg is unmistakable. It’s not just a muscle ache; it feels like something is wrong with the wiring of your body. This sensation is often caused by Radiculopathy, a condition where nerve roots are compressed or irritated as they exit the spinal column. Whether you feel it in your neck (cervical) or lower back (lumbar), this nerve pain can disrupt sleep, work, and daily life. But here is the good news: for most people, this isn’t a life sentence. With the right understanding and rehabilitation approach, you can quiet that nerve and get back to moving freely.
What Is Happening Inside Your Spine?
To fix the problem, you first need to understand what broke. Think of your spine as a highway system. The spinal cord is the main interstate, and the nerve roots are the exits leading to different parts of your body. When one of those exits gets blocked-usually by a bulging disc or bone spur-the traffic backs up. That backup creates inflammation and pressure on the nerve.
This pressure sends false signals. Instead of normal movement, your brain receives pain, numbness, or weakness. According to data from the American Academy of Physical Medicine and Rehabilitation, cervical and lumbar radiculopathy account for 95% of all cases. You aren’t alone in this. About 85% of people see their symptoms resolve within 12 weeks using conservative care, meaning surgery is rarely the first stop.
| Feature | Cervical (Neck) | Lumbar (Lower Back) |
|---|---|---|
| Common Cause | Herniated discs (under 50s); Degeneration (over 50s) | Herniated discs; Occupational lifting |
| Most Affected Nerves | C7 (57%) and C6 (27%) | L5 (49%) and S1 (43%) |
| Pain Pathway | Shoulder to fingers (thumb/middle finger common) | Buttock to foot (outer calf/big toe common) |
| Recovery Time | Average 11.1 weeks | Average 14.2 weeks |
Spotting the Signs: Where Does It Hurt?
Nerve pain follows a map. Doctors call these maps dermatomes. If you know which nerve is angry, you can predict exactly where the pain will land. This helps you communicate clearly with your physical therapist.
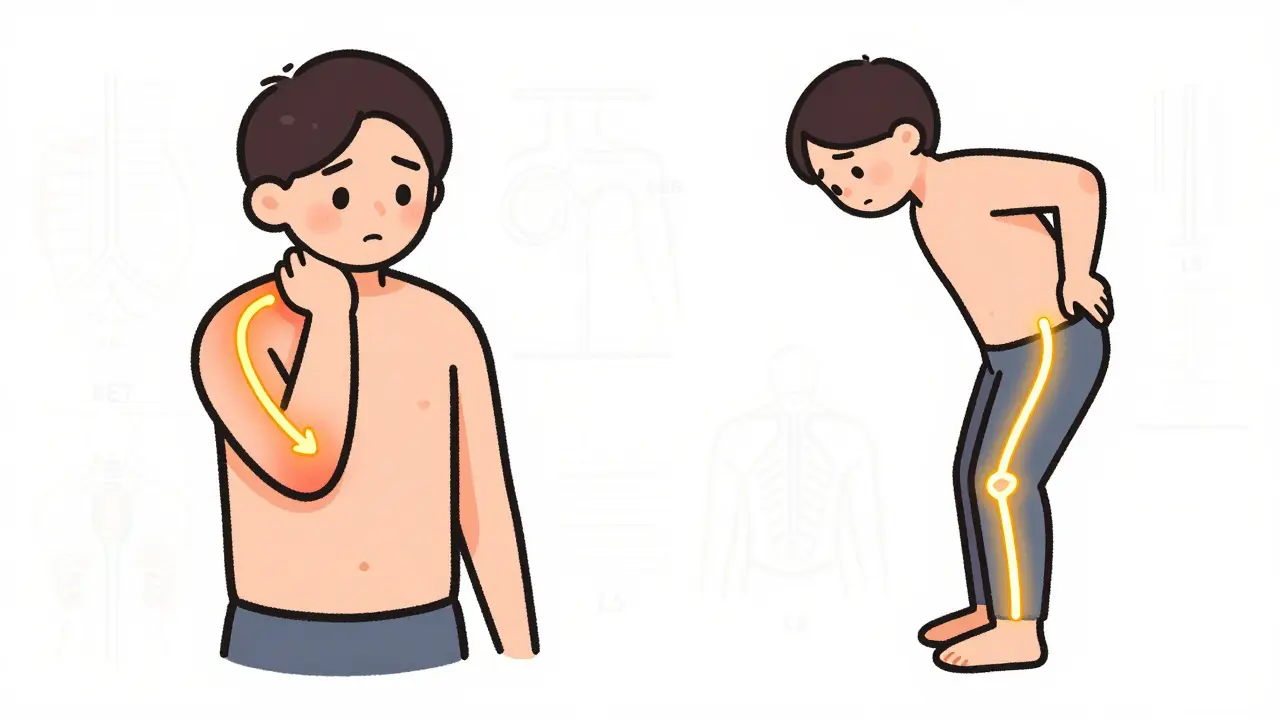
Cervical Radiculopathy: If the C6 nerve is pinched, you’ll likely feel pain radiating into your thumb and index finger, often accompanied by weakness in your biceps. The C7 nerve, the most common culprit, shoots pain down to your middle finger and weakens your triceps. Meanwhile, C8 issues affect your ring and little fingers, making it hard to grip objects firmly.
Lumbar Radiculopathy: Often called sciatica, this affects the lower body. Compression of the L5 nerve causes pain along the outer calf down to the big toe. A serious sign here is "foot drop," where you struggle to lift your toes. If the S1 nerve is involved, the pain travels down the back of the calf to the sole of the foot, and you might notice weakness when trying to stand on your tiptoes.
If you experience sudden loss of bladder or bowel control, or severe weakness in both legs, seek emergency care immediately. This could be cauda equina syndrome, a rare but serious condition requiring urgent surgical attention.
Why Did This Happen? Age and Lifestyle Factors
Your age plays a huge role in why this started. If you are under 50, there is a 90% chance a herniated disc is the cause. These discs act as cushions between vertebrae. When the soft center pushes out, it hits the nerve. However, if you are over 50, the story changes. Degenerative changes like spondylosis (wear-and-tear arthritis) and foraminal stenosis (narrowing of the nerve exit holes) account for nearly 80% of cervical cases.
Your job matters too. People who do heavy lifting or repetitive bending show a much higher risk for lumbar issues. Conversely, cervical radiculopathy is more often linked to acute trauma, like whiplash from a car accident, though poor posture at a desk contributes significantly over time.
The Rehab Roadmap: Step-by-Step Recovery
Most doctors recommend waiting 6 to 8 weeks before considering invasive procedures. During this window, physical therapy is king. Studies show it reduces symptoms in 68% of patients, compared to just 52% for medication alone. Here is how a typical evidence-based protocol looks.
Phase 1: Calm the Storm (Weeks 1-2)
The goal here is pain reduction. You might use NSAIDs like ibuprofen to lower inflammation. For neck pain, gentle cervical traction (pulling the head slightly away from the shoulders) can create space for the nerve. In the back, relative rest means avoiding heavy lifting but staying mobile enough to prevent stiffness.
Phase 2: Gentle Movement (Weeks 2-4)
Now you introduce motion. For the neck, chin tucks and scapular retractions (shoulder blade squeezes) help align the spine. For the lower back, McKenzie extension exercises-gently arching backward-are often effective for centralizing pain, pulling it away from the leg and back into the spine.
Phase 3: Strengthening (Weeks 4-8)
You start building armor around the spine. Isometric strengthening involves contracting muscles without moving the joint. This stabilizes the area without aggravating the nerve. Core stabilization becomes critical for lumbar patients, while deep neck flexor training helps cervical sufferers.
Phase 4: Dynamic Stability (Weeks 8-12)
This phase prepares you for real life. You practice movements that mimic daily activities, ensuring your spine stays stable under load. Most patients need 12 to 16 sessions of physical therapy to reach this stage effectively.
Home Habits That Make or Break Recovery
Physical therapy only happens an hour a week. What you do the other 167 hours matters more. Data shows that consistent home exercise adherence speeds up recovery by 47%. Skipping your exercises is the number one reason people don’t improve.
For neck pain, your pillow is crucial. A pillow that supports the natural curve of your neck prevents overnight strain. For back pain, ergonomic workstation modifications can reduce symptoms by 32%. Ensure your computer monitor is at eye level so you aren’t craning your neck, and keep your feet flat on the floor to support your lower back.
Avoid the trap of premature return to heavy lifting. Returning too soon causes symptom recurrence in 28% of cases. Listen to your body. If an exercise causes sharp, shooting pain, stop. Mild discomfort or stretching sensations are okay; electrical shocks are not.
When Conservative Care Isn't Enough
About 15% of cases don’t resolve with rehab alone. If you have progressive neurological deficits-like worsening foot drop or increasing hand weakness-you need immediate evaluation. Epidural steroid injections can provide short-term relief (2-6 weeks) for some, buying time for rehab to work. However, they are not a cure. Surgery is considered when pain is debilitating despite months of conservative care, or if there is significant motor loss.
How long does it take to recover from radiculopathy?
Most people see significant improvement within 12 weeks. Cervical radiculopathy typically resolves in about 11 weeks, while lumbar radiculopathy may take closer to 14 weeks. Consistent physical therapy and home exercises can speed this up by nearly half.
Can I cure radiculopathy without surgery?
Yes, approximately 85% of cases resolve with conservative management, including physical therapy, activity modification, and medication. Surgery is usually reserved for the 15% of cases with severe, persistent symptoms or progressive neurological damage.
What exercises are best for cervical radiculopathy?
Chin tucks, scapular retractions, and gentle cervical range-of-motion exercises are highly effective. Later stages include isometric neck strengthening and dynamic stabilization drills to support the spine during movement.
Is sciatica the same as lumbar radiculopathy?
Sciatica is a common term for lumbar radiculopathy affecting the sciatic nerve, specifically involving the L4, L5, or S1 nerve roots. While all sciatica is lumbar radiculopathy, not all lumbar radiculopathy presents as classic sciatica pain.
When should I see a doctor for nerve pain?
See a doctor if pain persists beyond 4-6 weeks, if you experience weakness in limbs, or if you have numbness in the saddle area (groin). Immediate emergency care is needed for loss of bladder/bowel control or severe bilateral leg weakness.